We live in a personalized world -- it's time to personalize care

A friend dog-sat for me recently and used my Netflix account. I’m a fan of smart comedies and sci-fi. My friend watches reality TV. After five days, my top recommendations for the next six weeks were shows like Love Island. It’s obvious why this happened — the Netflix algorithm noticed “my” behavior change, and thought I had developed a new guilty pleasure. It personalized recommendations based on my perceived behavior change.
We now live in the era of personalization. Scan a QR code at Starbucks to instantly order your venti almond milk cappuccino, two pumps vanilla, one pump hazelnut, with chocolate drizzle. (I’m a black coffee order myself.) Head to the Amazon app to see oddly intriguing items related to the last thing you searched. Checkout on Instacart and it will remind you that it may also be time to reorder paper towels based on the last time you bought them.
Personalized experiences are the new normal. McKinsey reports that 71% of consumers expect companies to deliver personalized interactions, and 76% of us get frustrated when we don’t receive them.
It comes as no surprise then that 76% of patients are frustrated when leaving their medical appointments, according to the AHIMA Foundation. Patients leave unsatisfied because they’re not receiving personalized care. Patients feel confused about their health, don’t get their questions answered, and feel like they need to do more research online.
And when consumers don’t like the experience they receive, a quick Google search will help them instantly find alternatives to spend their time and dollars. A Harris Poll showed that 69% of patients would switch healthcare providers for better services.
It’s time for the patient healthcare experience to match the consumer personalized experience.
It’s time for personalized care.
Personalizing care
When I co-founded Validic 10 years ago, personal health devices — glucose meters, blood pressure monitors, weight scales, activity trackers, and more — were going through a consumer technology evolution, making them connected, more usable, and more attractive to consumers. Validic saw an opportunity to use data from these devices to help people connect with their healthcare providers in a new way.
We have now connected personal health data for nearly 20 million people across hundreds of healthcare organizations. In that time, we have seen that the patient journey is not episodic, and people cannot be defined by their condition(s). People have different health goals, and need different levels of care at different times in their lives.
.png?sfvrsn=3a624d6d_1)
Understanding our consumer expectations around personalization and that we all have different healthcare needs at different times, we at Validic took a step back and wondered, “What would it look like to design a system that helps clinicians deliver personalized care for all patients?”
We recognized a few key things:
- Too much is already expected from our healthcare workers — we cannot ask them to do more. In fact, could we make their lives easier?
- Clinicians are frustrated by healthcare technology because it rarely works as advertised. Technology needs to be seamless, increase productivity, and do what it says it does.
- Most remote care pilots are clinically successful but operationally and financially unscalable. Healthcare labor shortages and costs are a top issue for every organization. Therefore, any proposed solution must be operationally and financially viable at scale.
We saw that the way to address the above is to help clinicians use everyday patient data in their everyday clinical workflow, the electronic health record (EHR). In the same way a clinician orders a lab test and views results in the EHR, a clinician enrolls a patient in a remote care program and views the remote data captured within the patient chart. They also receive alerts about abnormal or missing readings through the same communications methods already used in the EHR, such as secure messaging or in-basket messages. No additional logins. No extra steps.
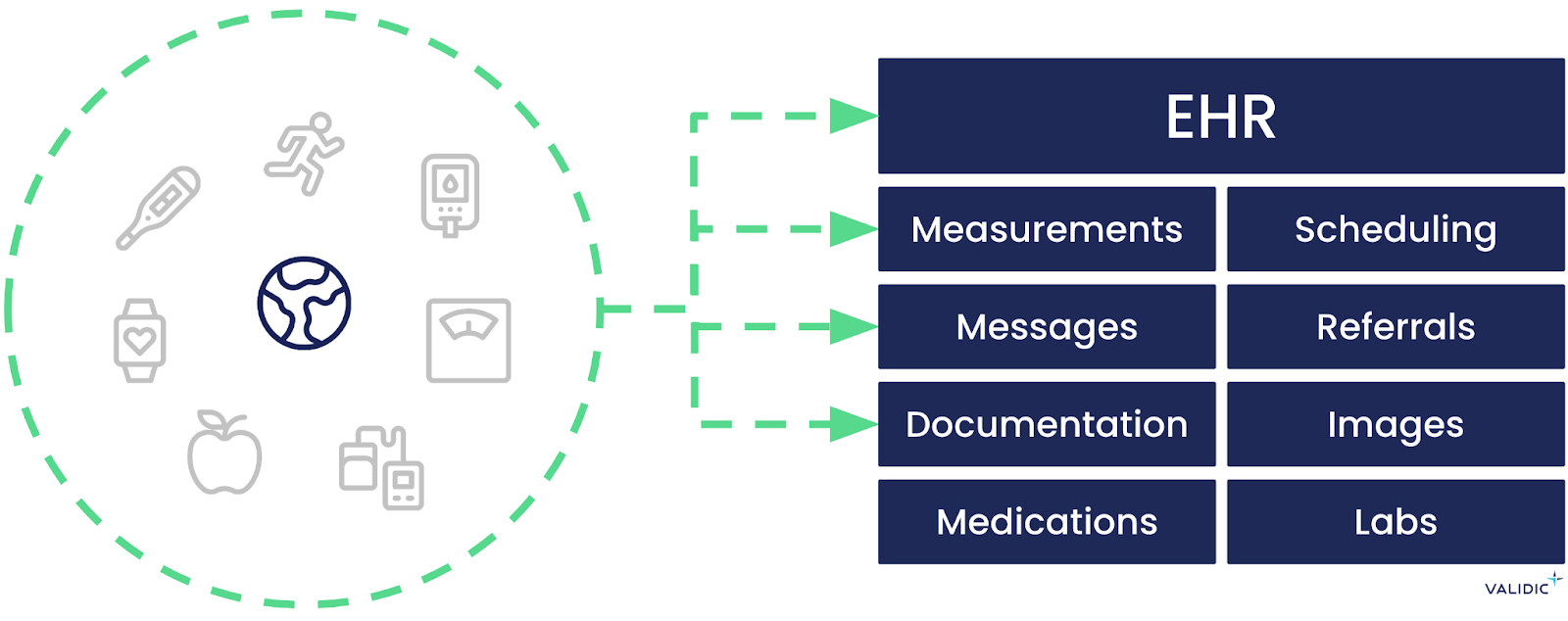
Personalized care in action
Steve Van, a Board Certified Patient Advocate, wrote an article on his struggles with type 2 diabetes, which also led to other health concerns. Steve was following his doctor’s advice, taking his medications, trying to eat healthy and exercise, but nothing was working. In fact, his health got worse, as Steve gained more weight and had to take more insulin. Like any rational consumer, he left his provider to find a better service.
“I sought out other medical providers and programs – finally landing on one at a different health system that made the difference. I volunteered for a study that included testing a new system of capturing your health data, specifically for people with diabetes. In this study, I was asked to follow my current blood glucose testing process and add the usage of an application to capture my data and share it with my care team. I would answer a few questions after the reading (for example: Is this reading pre- or post-meal?), and then my care team would receive the data automatically. I didn’t know it at the beginning, but this change would make all the difference.”
Author’s note: The program Steve refers to used Validic to bring data from the glucose meter into the EHR clinical workflow.
In Steve’s subsequent visits, the nurse could see Steve’s glucose meter data in his EHR patient chart. The data might have looked something like this (this is not Steve’s data):
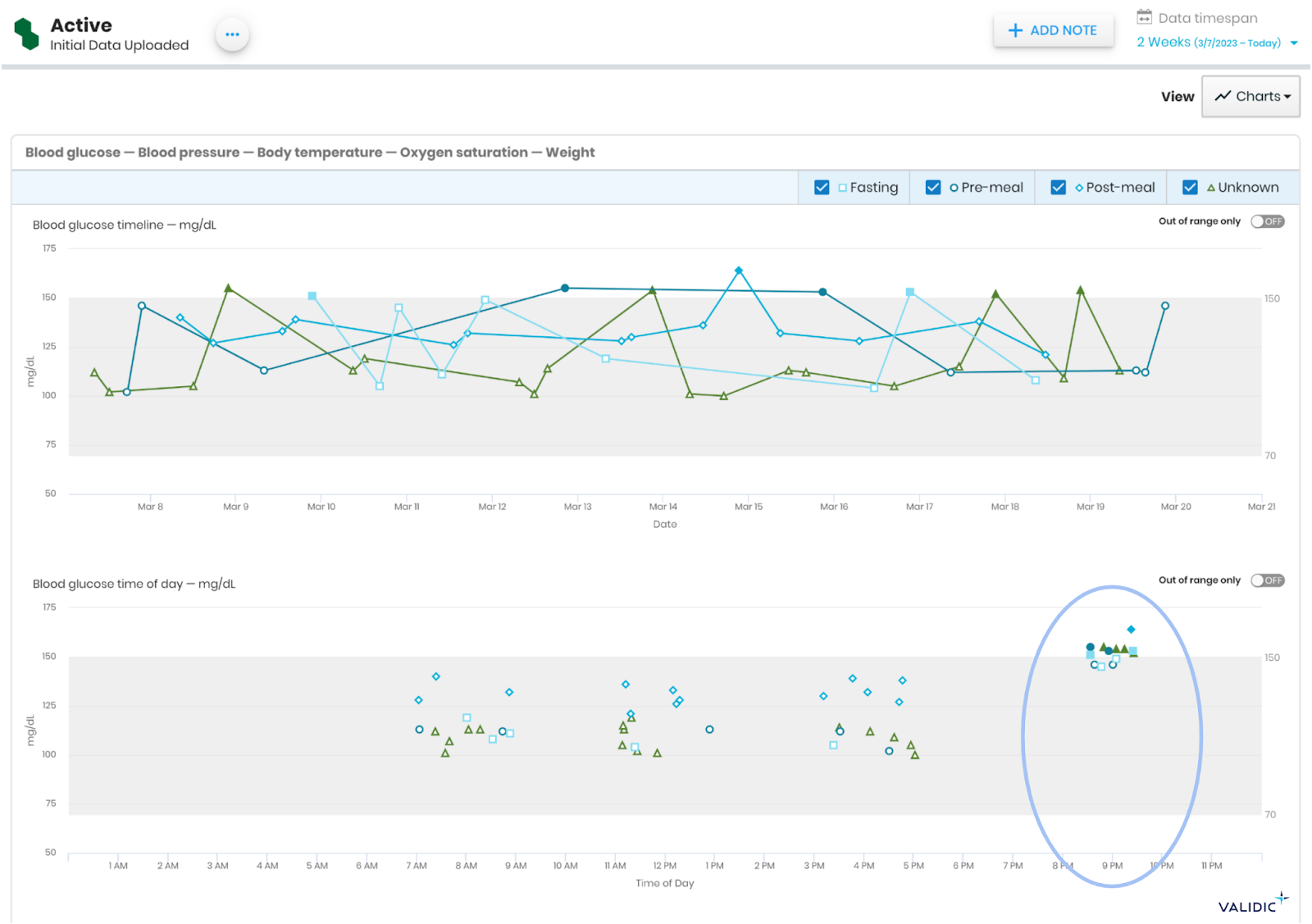
In this view, which is embedded in the EHR patient chart, a clinician can quickly see from the top chart that glucose readings are being tracked regularly. The bottom chart displays the same readings graphed over a 24-hour period. The clinician can see that the patient tracks regularly at certain times each day, but there is something going on in the evenings because the glucose levels are higher.
In Steve’s own words:
“Once I began sharing my data with my care team, they saw that my blood sugar levels increased between 8 and 10 p.m. most nights. The care team asked me what I was doing that could be increasing my blood sugar. I told them that during that time, my family and I would watch movies and all I was eating was a few handfuls of popcorn – a food I considered healthy. They informed me that popcorn is filled with sugar, and was the cause for the increase in blood sugar every night.
“This was my ‘a-ha moment.’ While this was a seemingly simple change, their suggestion to cut out the popcorn made a huge difference.”
Steve’s story has a happy ending. The data helped unlock a years-long dialogue with his healthcare team. Steve is now healthy and active, and he attributes his success to his healthcare providers using his own data to personalize his care.
Patient visits -- the old way vs. new way

Steve started like so many patients in the old paradigm of patient visits, where 76% of patients leave appointments feeling frustrated. In this “unsupported self-care” model, the patient shows up, and the nurse tries to make sure they get as much information as the patient can remember. Then the physician comes in and tries to quickly address the patient’s concern so they can move on to the next patient. This results in a gap between what the patient needs to do and what they actually end up doing.
Then Steve transitioned to the new personalized care model where, when a patient arrives for an appointment, their personal health data is already available in their chart. Now, the nurse confirms the information they see and discusses any details or questions they may have. The physician can quickly hone in on opportunities for patient education and tailored behavior guidance. The patient leaves feeling like they know what actions to take, and that they are on the same page.
Personalized care is better for patients and clinicians
As illustrated above, personalized care isn’t “another thing” for clinicians to do. Personalized care helps clinicians perform the tasks they are already doing better and more efficiently. In fact, in a Validic client survey, 88% of clinicians say these programs save them time, and 92% of clinicians say they feel like they are delivering better care.
Patients prefer being in these programs as well, as indicated by high patient satisfaction scores, improved care plan adherence, and better outcomes. 75% of patients say they feel like they are receiving better care, 76% of patients are still recording readings at least twice per day after 90 days in the programs, and 51% of patients report improved self management of their condition.

Validic supports successful personalized care programs from the largest healthcare organizations, such as Kaiser Permanente, to those helping the most marginalized patients, such as Delaware Valley Community Health, an FQHC in Philadelphia. The secret to the success of these programs is simple — the technology streamlines and better supports the clinician-patient relationship that has always existed and will continue to exist in healthcare. Validic integrates personal health data as a first-class citizen in the EHR to enable personalized care.
Personalized care exceeds expectations
It’s likely that your healthcare organization has tried remote care programs related to heart failure, diabetes, hypertension, or other post-acute conditions, and you’ve seen that patients like and succeed in these programs. But the challenge is: how can you scale the programs to cost-effectively and efficiently serve all your patients? At Validic, we’ve spent the last 10 years building a solution to answer that very question, evolving our platform and adapting to growing consumer expectations and market needs. As evidence of this, we support the largest centralized health system personalized care program in the U.S. at Kaiser Permanente.
Validic now offers an enterprise, tech-enabled solution to support healthcare organizations in delivering personalized care for patients across the entire care continuum, eliminating the need for multiple point solutions. In addition to our best-in-class EHR-integrated technology, we offer device ordering and shipping, kitting, friendly and engaging tech support, and onboarding support to help patients get set up and remain active in personalized care programs.
We are excited and proud to make personalized care the standard of care. Doing so will help overburdened clinicians care for their patients more efficiently and effectively in their current environment. It will help patients feel heard and understood, like they belong with their healthcare providers, and help them live their best life.